I was hoping my health would have improved after experiencing chronic pain complications after returning to work following my 8th surgery; but alas, there has been none.
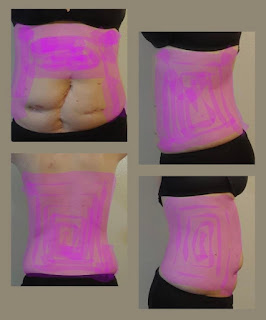 |
| Where I've Been Having Chronic Pain since 9/13/21 |
Not only has my pain continued throughout the majority of my torso, since 9/28/21 my incisions have
started feeling as though they are ripping from the inside out whenever my abdominal muscles are strained or stretched in the least bit.
I returned to the surgeon on 10/6/21 and he decided to order another CT scan without contrast as my pain hadn't improved. My latest CT scan on 10/14/21 revealed a small hiatal hernia and everything else remained the same. I was distraught upon reading these results. I fully expected to require additional surgery in my lifetime but I didn't expect the possibility of another surgery so soon. I contacted the surgeon's office asking to speak to him about the CT results as I was very upset. He contacted me via phone that afternoon and the information I was provided was even further upsetting to me. I had been crying nearly non-stop after reading my CT results and was actively crying when he called me. The surgeon told me that he believed:
- My hernia wasn't causing or contributing to my pain even the upper stomach pain
- My pain isn't new
- I've had this hernia all along
- He was releasing me to my GI and PCP as he has nothing to offer me or idea what is causing my pain
I wasn't fully processing the information he stated and only managed to repeat the exact things he said but in a question form. To this, he simply repeated the same information without any elaboration of his conclusions or advice for going forward. Afterwards, I realized that the information he stated didn't make sense. The more I thought about it, the more I became enraged. The next day, I left a voicemail for his office explaining that I was confused by his statements for the following reasons:
- Upper stomach pain can be a pain symptom of hiatal hernia
- The pains I've been reporting since 9/13/21 are new, I didn't have them before surgery and the issues I was having prior to surgery, I'm no longer having
- I have had multiple, repeated testing that includes the ones used to diagnose a hiatal hernia and none of those tests ever showed a hiatal hernia until this one
His Medical Assistant called me back and stated "He told me that none of this changes anything, he has nothing surgically to offer you but if you want to see him in the office to discuss it, you can".
This further enraged me as I felt my trust in this doctor had been betrayed, my concerns and questions dismissed, and I felt frankly abandoned. I thought he understood my medical complexity and that my body has never followed the medical textbook explanations for anything. I felt he had indicated he would follow through with trying to identify the issues I've been having since surgery and now, he was giving up on me. Furthermore, why should I pay this surgeon a copay to finally get answers to the questions I posed when he should have explained his conclusions when he was on the phone with me the day before especially when I'm going to have to pay a copay to consult with my GI and PCP anyway. I figured, I might as well obtain a second opinion from another surgeon, pay that person my copay, and have all my questions answered in one. And, at this point, with confidence and trust lost in this surgeon, I wouldn't feel able to fully believe anything he says going forward.
I immediately followed up with my PCP, GI, and sought a second opinion from another surgeon.
My PCP advised she didn't believe my hernia was causing my pain due to the large scale of my pain not being consistent with symptoms of hiatal hernias. Instead, she thought my pain may be caused by gassiness from my probiotic or esophageal spasms. She advised to stop my probiotic for 1-2 months to determine if my pain would improve. I had stopped taking my Bentyl after surgery as I no longer have been having the abdominal pain it was controlling but resumed the Bentyl as it may help with esophageal spasms. I have not noticed any improvements to my pain with either of these medication changes thus far.
My GI ordered lab and stool tests as the surgeon hadn't checked my blood tests again after my pain started, only before my pain started. Tests showed that my liver and pancreas enzymes are high, white cell blood count low, and there continues to be blood in my stool and the calprotectin levels measuring inflammation in the GI doubled since 8/3/21 - from 58 to 117. Both of these levels remain in the borderline range, however, 120 is the threshold for elevated. He also ordered an abdominal ultrasound, however, no issues were identified by the ultrasound. He suggested the new pain may be due to adhesions. Although, I don't understand why abdominal adhesions would cause pain everywhere other than the abdomen especially considering I just had adhesions removal and the adhesion pain I had prior to this, has stopped. He started me on Carafate for possible Bile Gastritis and I will see him in the office for a follow up on 12/2/21. I remain in regular contact with him and his office though, so he may order additional tests in the meantime.
My Nephrologist advised she believes my torso pain is caused by dehydration and my high liver enzymes are likely due to my medications. Neither of these suggestions make sense to me and my GI reviewed my medications following my test results for possible contraindications with the liver and found none.
I also scheduled with another surgeon. I obtained the images of my 3 CT scans from this year for him to review and I brought all my paper medical records I have for him as well. The moment I stepped into his office building, I began to cry and continued to do so until he met with me. This was due to my high level of
fear and mistrust in new medical providers due to my medical trauma. I felt confident in him prior to our meeting as his reputation as a surgeon is well known and a friend is his patient for hernia repair as well. He spent an hour reviewing my records and talking with me. While he agreed that I am a complicated medical case he explained to me that:
- He isn't convinced I even have a hernia. If I do have a hiatal hernia, it is "tiny".
- He doesn't believe my possible hiatal hernia is causing me any issues
- He doesn't recommend surgery at this time as he doesn't believe it would benefit me and would only worsen my health issues
- He believes I have recovered well from the surgery itself and my incision pain is likely due to adhesions. My abdomen is also not likely to ever feel "normal" due to all the surgeries I've required so the abdomen issues I'm having are likely to be my normal. (Honestly, I figured as much so I wasn't surprised)
- He doesn't know what is causing my pain and believes my other doctors are "throwing darts" but recommends scopes if gastritis is suspected and to have a Bravo pH test done at the same time to measure my stomach acid
With my 2nd opinion complete, I feel comfortable in trusting that my possible hernia isn't the issue and I can now relax about the hernia. I don't believe my probiotic or dehydration is the culprit. I don't believe I'm having esophageal spasms and perhaps it is bile gastritis but not convinced there either. Honestly, I'm hoping the Carafate isn't effective as I don't want to take this medicine for the remainder of my life.
I'm required to take the Carafate 1 hour before meals or 2 hours after meals or I will have an intestinal blockage, which I am already prone to due to adhesions. I typically only eat 1 meal a day in the evening and it is usually only when I'm with
Mike for dinner 4-6 times a week. Without him, it's debatable if I will eat anything for the day. When I do eat outside of my daily meal, it is typically a very small snack and often it is late in the day. Therefore, timing when I can safely take the Carafate has been a nightmare. I also am beginning to think the Carafate may be causing me to feel worse. I've noticed I've started feeling feverish (even though I don't have a fever), nauseated, sick to my stomach, symptoms of low blood sugar, and the like sometimes within 30 minutes of taking it.
I continue to have pain from pressure placed on my abdomen including from clothes or bending. A physical abdominal exam causes severe, post surgery like pain for 1.5-2 days after the exam. I haven't noticed any improvements to my torso pain since it began in mid September, but I do believe I am starting to tolerate it better most days. I suppose that's something. Unfortunately, OTC pain medications are no longer dulling the pain and having my muscles massaged causes intolerable pain. I don't want to start taking prescription strength pain medications for multiple reasons either. At this time, I just hope the pain will improve over time or I will continue to at least improve in my toleration.